 |
| Dr. Dineshi Liyanage, medical director of palliative care services at Clovis Community Medical Center and Fresno Heart & Surgical Hospital. |
Dr. Liyanage: It is estimated by the Alzheimer’s Association that in 2016, 5.4 million Americans suffer from the disease. The number is expected to triple by 2050 with the increasing population of baby boomers. It is the only disease among the ten most common causes of death in America that cannot be cured, prevented or slowed in its progression. Age is the greatest known risk factor for this disease. An estimated 32% of people over 85 are afflicted. This is a rapidly growing demographic, so we’re going to see many, many patients. In order to meet their needs, there will be increasing demand for palliative care specialists. (Palliative care specialists work with patients and their families to educate them on the diagnosis, illness trajectory and help them determine their goals of care. They also help them evaluate treatment options in light of their values and help improve their quality of life while managing the symptoms of complex, chronic and terminal conditions.)
Q: Are there predictable patterns to the progression of Alzheimer’s disease?
Dr. Liyanage: The duration from diagnosis to death is typically four to eight years. It’s a terminal condition, but it progresses over quite some time. The cognitive, physical, personality and behavioral changes place demands on the caregivers and increase exponentially as the disease progresses. At the end-stage patients become bedridden, incontinent, speech becomes limited, they are dependent for bathing, dressing and feeding and have recurrent infections. Typically they suffer from urinary tract infections and pneumonia which is often related to difficulty in swallowing which leads to aspiration of food, liquid or their own saliva. They may have bed sores and painful contracted limbs that are fixed in position and not movable.
While the physical progression is predictable, it’s difficult to predict how each individual may change in terms of personality. Some become combative and paranoid. Some are sexually inappropriate. Some patients remain sweet and others may remain their ornery selves all their lives. We see others who were perfect gentlemen before the disease, later start to use profanity. This is part of the caregiver burden I warn the family about. They need tremendous support. They can experience anxiety and depression themselves and may neglect their own health.
Q: What kind of conversations should families be having when someone is first diagnosed with Alzheimer’s?
Dr. Liyanage: Before the disease progresses it’s important to talk about wishes – how one would want to be taken care of. Families will need help to understand the natural course of the disease and help in making educated choices about potential medical interventions along the way. When people are first diagnosed they may be able to make those decisions for themselves. However, at the point where a decision about a feeding tube or use of a respirator is needed, the patients are often so cognitively impaired that they can’t be involved. It is a gift to the person responsible for making those decisions to have had prior discussions with the patient so that the decisions are aligned with the patient’s values and expectations.
Q: What are the main things families should be talking about and thinking about ahead of time?
Dr. Liyanage: When I explain the progression of the disease, we talk about the medical interventions they might face along the way and the choices they will have:
- To use a Foley catheter or diapers
- To use a feeding tube
- To treat other diseases as they arise
- To use antibiotics
- To do CPR or have a “Do Not Resuscitate” order
Q. What about the choice between a Foley catheter or diapers?
Dr. Liyanage: When patients are incontinent the resulting moisture can contribute to bed sores. A Foley catheter can protect the skin, however, some patients may be uncomfortable with a catheter and others may try to pull it out in their confused state. It’s a matter of weighing the risks and benefits in each case.
 |
| Feliciano Cruz and his ailing father, Mario Cruz, talk with a palliative care nurse and social worker about the elder Cruz’ preferences for care at Community Regional Medical Center. |
Dr. Liyanage: Culturally there is so much value on food, so when the patient is unable to swallow, the family may feel they have to feed them in order to feel like a good caregiver and avert the commonly held notion of suffering from “starvation”. People don’t understand that inability to swallow and losing appetite are signs that the end is near. When a feeding tube is placed, the patient isn’t tasting the food or getting pleasure from it. There is nothing social in the sense of being able to break bread with the family. Often the patients don’t understand why there’s a tube in them, they get agitated and try to pull it out, which can lead to infections and trauma. Sometimes to prevent that patients will be placed in restraints. Where is the quality of life for that patient? I’ve seen patients with feeding tubes who have had a painfully prolonged course lying in bed, prone to bed sores, limbs contracted, and getting infection after infection. Tube feeding is typically brought up when a patient can no longer swallow safely. However, tube feeding does not eliminate the risk of aspiration of saliva or the tube feeding itself. Repeated aspiration leads to repeated attacks of pneumonias.
There are many families who think that not eating at the end of life is painful, but when they understand the natural process, they are often comforted. When a patient ceases eating or drinking due to disease, the body releases its natural pain-killers called endorphins that reduce discomfort. They just aren’t hungry.
Q. What other disease conditions are Alzheimer’s disease patients likely to encounter?
Dr. Liyanage: The patients often have multiple other medical conditions. Some have cancer, kidney disease, heart disease or other diseases common in the elderly. In palliative care we look at the whole person. At what point in the progression of disease does it make sense to stop treatment? Do you give patients chemotherapy if they can’t articulate that they are feeling the side effects? They could be more prone to have serious complications which could potentially shorten their lives.
Q. Using antibiotics seems like a typical medical practice. Why is it different for a patient with Alzheimer’s disease?
Dr. Liyanage: Families don’t realize that infection is part of the illness trajectory, so in their minds they separate them as though there is dementia and then there is an infection. They are in fact tied together. Infection is the most common and expected cause of death. As the body gets weaker, the immune system also becomes weak. As a result, the patient becomes more and more prone to infection. Typically patients will have recurring urinary tract infections or pneumonia. They may get antibiotics, but then another infection occurs or the infection just gets repressed and it flares up again. For instance, when a patient keeps aspirating, say on his saliva, antibiotics will have a hard time controlling the resulting pneumonia.
Antibiotics are treated almost like candy. People just take them without realizing there are significant implications in taking them. You have to ask if it is actually going to be of meaningful benefit. Antibiotics might perk patients up for a bit but really that infection is often a sign of the end stage. Not treating the infection would be consistent with the goal of letting the disease take its natural course.
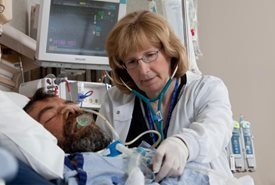 |
| Community Regional Medical Center nurse Diane Huffman cares for a patient in intensive care who is on a respirator. |
Dr. Liyanage: If you describe CPR and its burden on elderly patients, families see it differently. I talk about chest compression and how in elderly patients their ribs are likely to break and how it’s painful. Electric shock with a defibrillator is also painful. Breathing tubes and breathing machines can be uncomfortable. Even if we did all of that, in light of the underlying disease, it’s unlikely to work and more likely to result in a painful and traumatic death.
Q: How important is it to have these kinds of conversations early in the diagnosis?
Dr. Liyanage: I find with families who have already gone through putting in a feeding tube, it’s much more difficult to stop the feeding. There may be a sense of guilt for having put the patient through it in the first place. For some it becomes the norm, to treat frequent infections with antibiotics, keep feeding with a tube, and to keep trying to prevent or heal bed sores when the patient mentally is no longer aware. Ideally the conversation should happen as early as possible in the course of the disease, to make sure that the family is educated on the pros and cons of each intervention.
Many times patients’ families feel awkward talking about death and dying and end of life wishes. That conversation can be facilitated by a physician saying, “This is an important topic that we need to address to make sure that our care plan is consistent with the goals and values of the patient and family.”
Q: What’s the number one thing people can do to prepare?
Dr. Liyanage: I highly encourage patients to complete Advance Directive forms. They should also speak to their surrogate medical decision maker about their views on quantity vs quality of life and other values. I tell patients it’s a gift to their family which can relieve some of the burden in making medical decisions as they can have a clearer understanding of the patient’s wishes. Some people think it’s morbid. They have the mentality that death doesn’t happen.
If people accept that death is inevitable and take steps to ensure that their end of life care wishes are followed when they are incapacitated, it may provide peace of mind to the patient and the family. In the meanwhile, care can be tailored to help us live our lives to the fullest, in the way that is most meaningful to us.
Erin Kennedy reported this story. Reach her at MedWatchToday@communitymedical.org


