Homeless patients who are hospitalized, treated and then discharged back to the streets have higher rates of readmission to hospitals compared with those who have established residences. To help better manage their recovery, Community Medical Centers and others created the Fresno Medical Respite Center, a nearly four-year-old “bridge” residence at the Fresno Rescue Mission that so far has assisted nearly 150 men and women.
Without the Medical Respite Center, 60-year-old Jose Sanchez likely would’ve had to spend a few more days in the hospital recuperating from a broken right leg, cuts and bruising he suffered when a car side-swiped him while he was out riding his bike. Sanchez lives intermittently in a downtown auto repair shop and has no family in the U.S. to help him in his recovery. He’s grateful for a soft bed, a safe place to stay and the medical follow up he’s receiving.
“Oh, I have been treated very well. Very well indeed. And they even gave me that,” he said pointing to the metal walker he got after his stay at Community Regional Medical Center. “I can walk now, and this helps too.” He said of the leg brace that was fitted for his fractured leg.
The 8-bed Respite Center is based on home-like models successfully implemented elsewhere in California, providing shelter, food, follow-up care and social services. Patients there have been recovering from such things as hip transplants, pneumonia, burns and other wounds. Respite center partners include: Community, Clinica Sierra Vista, the Hospital Council, St. Agnes Medical Center and Kaiser Permanente.
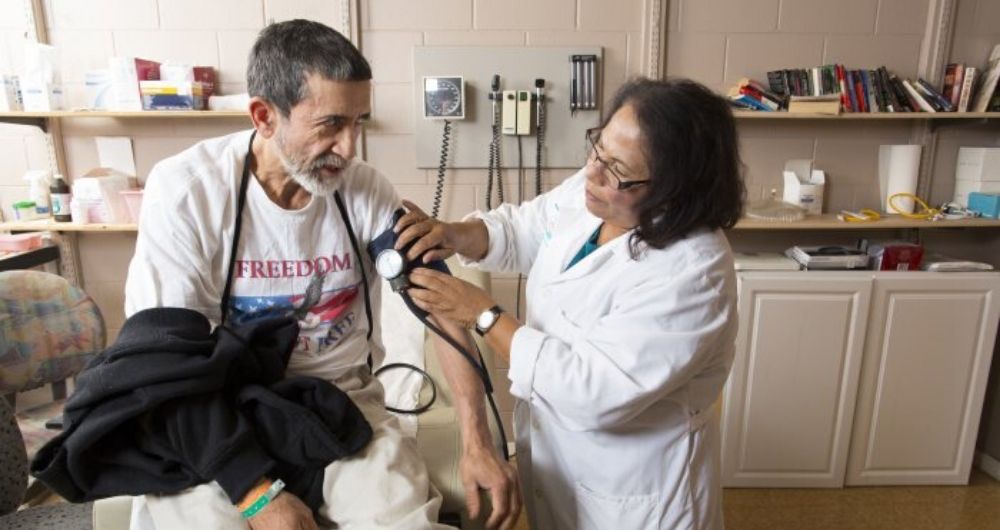
“These patients would not survive outside in the cold or in the heat,” said Blanca Tristan, a nurse practitioner with Clinica Sierra Vista, which evaluates patients before admission and provides follow-up.
 The Hospital Council estimates the program has saved hospitals near $6 million in unnecessary extended hospitalization or repeat hospitalization costs. Homeless people tend to stay in hospitals 4.5 days longer than patients who have other options for recuperative care.
The Hospital Council estimates the program has saved hospitals near $6 million in unnecessary extended hospitalization or repeat hospitalization costs. Homeless people tend to stay in hospitals 4.5 days longer than patients who have other options for recuperative care.
“Patients stay anywhere from a few days to a few months,” said Lynne Ashbeck, vice president at Community Medical Centers who helped facilitate the center’s creation when she was regional vice president of the Hospital Council of Northern and Central California. “Our goals are to ensure their recovery and connect them with the services they need in the community ... Our community is better today because of this resource.”
Alma Martinez, Community Outreach Specialist, and John G. Taylor, Public Affairs Director, reported this story. Reach them at MedWatchToday@Communitymedical.org