Lupus is a complicated and often difficult-to-diagnose disease that affects an estimated 1.5 million Americans — women more than in men. Symptoms usually start in early adulthood, from the teen years into the 30s.
What’s tricky about lupus is that it can go undetected for months or even years because it causes different symptoms in different people and can be confused with what doctors might expect with COVID-19 patients.
In some patients, the symptoms are mild. In others, they can be life threatening.
What lupus can look and feel like
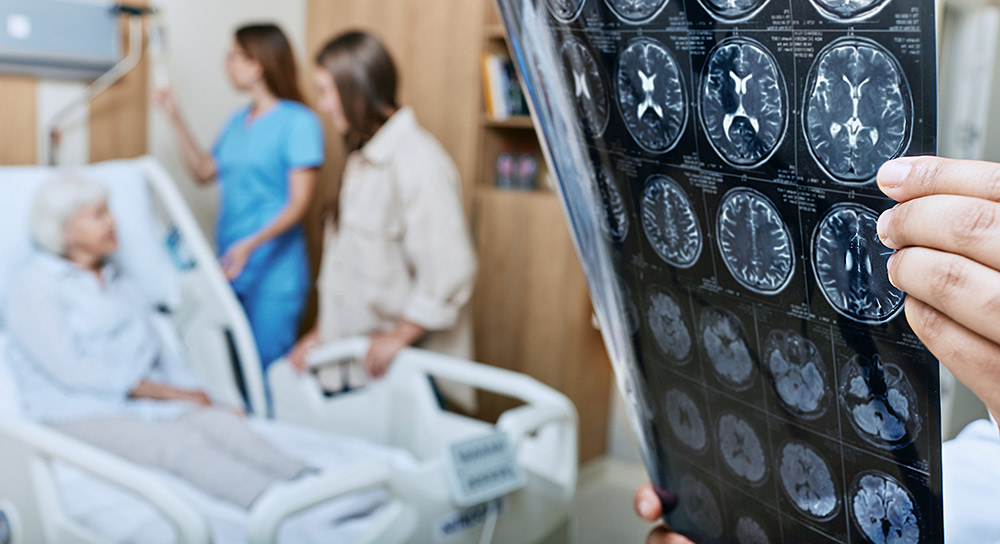
A 57-year-old white female was recently admitted to a Fresno hospital with shortness of breath and low oxygen levels. Until just a few weeks earlier she was walking fine and working full time — now she couldn’t walk to the bathroom without oxygen.
 A chest image showed pneumonia and inflammation related to changes in her lungs. She was started on antibiotics while the doctors tried to improve her oxygen levels. They also called Dr. Manisha Mittal, a rheumatologist (a specialist in conditions of the muscles, joints and bones) who sees patients at Community Medical Centers' hospitals and also practices integrative medicine at Moksha Holistic Center.
A chest image showed pneumonia and inflammation related to changes in her lungs. She was started on antibiotics while the doctors tried to improve her oxygen levels. They also called Dr. Manisha Mittal, a rheumatologist (a specialist in conditions of the muscles, joints and bones) who sees patients at Community Medical Centers' hospitals and also practices integrative medicine at Moksha Holistic Center.
Dr. Mittal asked the patient some specific questions and learned that over the past few months she had been experiencing joint pain, dry eyes and mouth, and sores (ulcers) in her mouth. When her lupus workup came back positive, the patient was switched to immune-suppressing medications and steroids used to treat lupus. Within two days she was off oxygen and fully functional, said the doctor.
‘The great mimicker’
Lupus is a chronic, or long-term, disease that can cause pain and inflammation in any part of the body. It’s an autoimmune disease, which means that your immune system — the body system that usually fights infections — attacks healthy tissue instead.
Most patients will have times when the disease is active, followed by times when the disease is quiet — referred to as remission.
That makes it harder for patients to know when to seek treatment and for medical professionals to pinpoint what’s wrong. “I call lupus ‘the great mimicker’ because it can present in a lot of nonspecific ways, including feeling like you’ve been hit by a bus, low-grade fevers, fatigue, achiness in the joints, hair loss or oral ulcers,” said Dr. Mittal.
These symptoms are often misdiagnosed — sometimes for years, she added.
Slowing and managing lupus
Rheumatologists can treat lupus with a number of medications that can effectively slow the progress of disease. However, therapy is often tailored to the individual's particular symptoms.
Right now, there’s no cure for lupus. Early diagnosis, as well as avoiding triggers for the disease such as excessive exposure to the sun, can aid in the management of lupus, according to the Lupus Foundation of America.
“The good news is that with the support of your doctors and loved ones, you can learn to manage lupus and likely return to your normal life,” said Dr. Mittal.
Wear purple to show support
May is Lupus Awareness Month, and May 10 is World Lupus Day. Both observances bring awareness to the disease and encourage more medical research on its origins and treatment.
The color purple is associated with lupus so during the month you may see healthcare workers, patients and their families wearing purple to show their support for those afflicted with this somewhat obscure autoimmune disease.
You can learn more about lupus at the American College of Rheumatology, the Lupus Foundation of America or the Lupus Foundation of Northern California.