Andrew Caquias considers the morning he fell asleep at the wheel on his way home from work as a hospital security guard a blessing in disguise.
He veered off the freeway, hit a guardrail, went over a steep embankment and smacked into an eucalyptus tree going 80 miles an hour. When the first hospital he was taken to found two brain bleeds in a CT scan, Caquias was transferred for a higher level of care to Community Regional Medical Center, where he works.

After two days in the hospital, he was discharged home, but nausea and dizziness sent him back to the emergency room where additional scanning was done with an MRI machine. The more detailed image revealed a brain tumor pressing against Caquias’s brain stem in an area that affects movement and vision.
Caquias had been ignoring his increasing troubles with balance, unexpected falls, blurry vision and sudden migraine headaches. “Prior to my accident, I noticed I had a loss of appetite and problems with balance and I was tired, but I associated it with having two jobs. Without me going to the doctor and me being the tough guy that I am, I might have never found it,” he says. “I’m grateful that the accident exposed the brain tumor.”
More brain surgeries than any other Valley hospital
He’s also grateful it was discovered by the region’s top neuroscience team, who performs 41% of the brain cancer surgeries in a seven-county region in the Valley. Last year, Community Regional performed 670 brain surgeries.
Community Regional’s Bob Smittcamp Family Neuroscience Institute is uniquely equipped to handle cases like Caquias’s. It includes a 20-bed neuroscience critical care unit and a 52-bed neuroscience unit dedicated to spine and brain patients, as well as a combination of neurosurgical technologies and services offered only in a few places in the state. The technology includes the Gen4 CyberKnife®, two 64-slice CT scanners, new neuroscience operating suite, three-dimensional real-time surgical imaging equipment and faculty surgeons from UCSF Fresno.
Community has long been dedicated to caring for brains and spines, becoming one of the first 17 hospitals in the nation to open a hybrid operating suite with biplane technology in 2014 so surgical teams can go from a minimally invasive procedure to a full open cranial or spine surgery within minutes. A second hybrid operating room opened in 2017 increased that capacity.
Community Regional is also one of only 13 Level 1 trauma centers in California, and the only one between Los Angeles and Sacramento. Serving a 15,000-square-mile region, besides having neurosurgeons, the Table Mountain Rancheria Trauma Center has specialists in heart, trauma and other surgeries available 24/7.
Neurosurgeon Nicholas Levine agrees with his patient: “Sometimes things happen for a reason. He was very fortunate and walked away with limited injuries from his car accident, but he ended up finding something no one expected.”
Most common brain tumor is usually not cancerous
The MRI at Community Regional revealed a meningioma. “Most of the time it’s a benign tumor in the covering of the brain,” explains Dr. Levine, a Community Health Partners specialist with Community Neurosciences Institute. “In Andrew’s case, it was growing and pushing on his brain stem and causing compression of the brain at the back of his head. And that caused him to have dizziness and balance problems and really accounted for all of the symptoms he was having.”
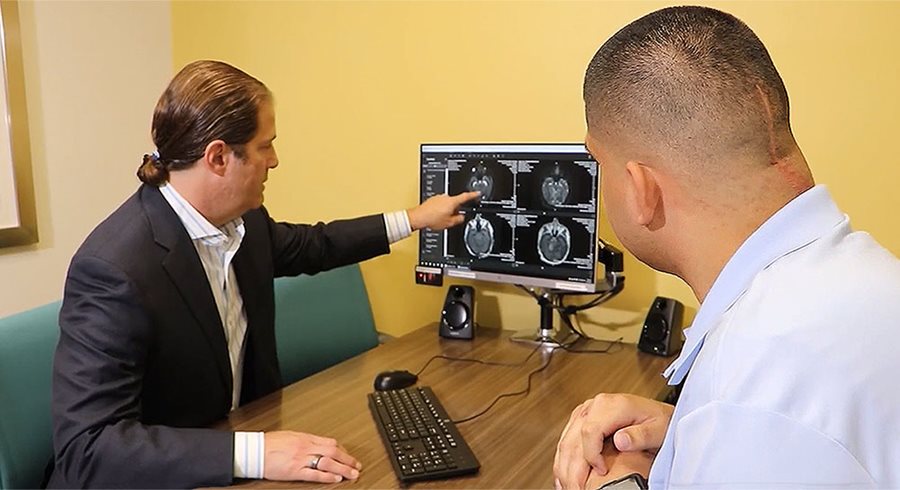
Dr. Levine explains further: “Meningioma is the most common brain tumor we find, but it’s still rare with only one out of 200,000 people getting them. And about 90% are totally benign. It’s really about where it grows and how quickly it grows.”
Meningiomas occur more often in older people and are usually a spontaneous growth, not connected to any specific lifestyle risk factors or environmental exposures. In rare cases there’s a genetic cause. Often they’re slow growing and take years to cause serious problems.
Dr. Levine determined the tumor big enough and causing enough symptoms that it needed to come out, but there was time for Caquias to absorb the news, talk to his family and prepare for surgery.
Neurosurgery removes golf ball-sized mass
“He explained that my case was really urgent based on the size of the brain tumor — the tumor was as big as a golf ball and that’s why it was pressing on my brain stem,” Caquias says. “Dr. Levine explained everything to my mom and said if this was his kid, this is what he would do.”
After surgery, Caquias spent some time in intensive care and two weeks on the neuroscience floor at Community Regional. Then he was moved to the Leon S. Peters Rehabilitation Center in the hospital for more therapy.
Caquias worried that he might not regain all his mobility or thinking skills. “He removed the whole tumor – 100%. It was scary because I didn’t know there would be deficits from that … It was a long road to recovery and I was still working with a walker when I left the hospital. PT (physical therapy) helped, and speech language therapy helped.”
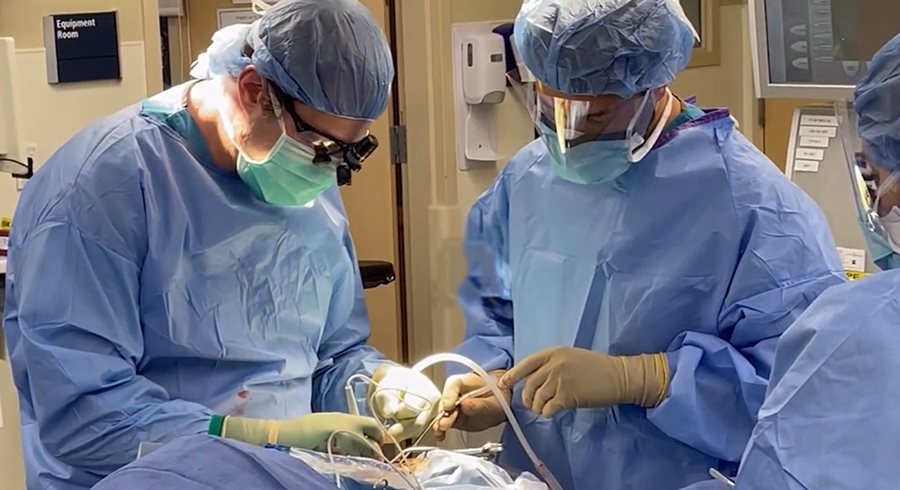
Dr. Levine assures Caquias that, “It takes up to a year really to recover.” He adds, “When someone has this operation we hope they are at least where they were before the operation. He may have some balance issues, but the dizziness is gone.”
Caquias is using a cane now, a few months after his operation, and working on recovering fully with hopes of becoming a law enforcement officer someday.
“I’m grateful to Dr. Levine and the neuro and ICU staff; they all did a great job,” says Caquias. This changed my outlook on life a lot. I really appreciate things a lot more.”
Caquias is also grateful for the crash that totaled his car and landed him in the hospital. “In my family we call the accident a miracle in disguise. God works in mysterious ways.”
Community’s Commitment to Making Care Accessible
Our mission of improving the health of our region is dependent on continually enhancing our medical expertise and investing in research and technology so everyone, regardless of their circumstance, has access to top-level care. We aim to rank among the nation’s top hospitals in delivering measurable quality care and investing in best practices and innovative technology. Read more stories.


.jpg)
